|
Why Cash-based PT?
A common barrier to someone seeking care at Goodman Performance Therapy (GPT) is “If I’m not using my insurance for physical therapy services, then I’m wasting my money. “ There are several factors to consider when providing this answer. Cost To understand cost, lets look at some definitions of your insurance plan. Deductible - amount of money paid for covered healthcare services each year until health benefits take effect. Co-insurance - a percentage of a healthcare services you pay AFTER your deductible has been met. Maximum out-of-pocket - the maximum amount of money that you have to pay for healthcare services in a plan year (deductible + co-insurance). Copays - a flat fee you pay at the time of a healthcare service (office visit for example). I recently heard a patient say “Do you know how much physical therapy costs?” when looking into treatment at another local clinic. I think the simple answer is no, most people don’t realize the true cost of receiving physical therapy. Charges for PT are based on units, which in simple terms describe what is being performed (i.e. Therapeutic exercise, Manual therapy), and are roughly billed for every 15 minutes that this procedure is performed. So for a 45 minutes appointment, typically 3 units will be billed and if you end your session with ice and electrical stimulation this adds another unit. At some clinics, the charges can be over $150 PER UNIT! So for your one visit, the clinic may be submitting over $600 charge to your insurance company, if not higher based on how long you are there. The twist that complicates medical billing is the negotiated rates that the insurance company has with the companies providing the services. That $600 charge will be negotiated down by a contracted rate. This rate varies by insurance company and is specific to companies providing the services. It is also not usually known until you receive a statement in the mail asking for payment. Unfortunately, these statements are delayed and you could receive all or most of your treatment before the insurance company is even billed. Your statement may come months after you finish your care. So what does this mean? Often, unfortunately this means a SURPRISE BILL. Most companies will ask for a prepayment toward these charges based on an estimate. For someone that hasn’t met their deductible/out of pocket, this prepayment per visit can be $300. Alternatively, in a cash-based PT clinic, the charge for the visit is paid prior to the treatment and there is no worry about a surprise bill afterwards. When working in a traditional PT clinic, a therapist is often torn between doing what’s right for the patient from a treatment perspective and meeting productivity standards set by the employer. These productivity standards are typically a set number of units the therapist is supposed to bill each patient, a total number of units per hours worked in a day, or a combination of both. Productivity is often linked to performance reviews, bonuses, and staffing decisions for the clinic. So if the therapist dosen’t want to have a sit down meeting with their boss, wants to get a bonus, or wants to keep layoffs from occurring they are pressured to get your units in a day. Another cost consideration is the physician visit. Ohio is a “direct access” state, which means patients can seek the care from a physical therapist without a physician prescription (you don’t need to see your doctor before going to PT!). However, most insurance companies require you to have a prescription from a physician before paying for PT services. In a cash-based system, you aren’t required to see a physician prior to scheduling PT. When seeing a skilled PT directly, the therapist has the skills to determine if treatment is warranted or a physician is needed for possible medication intervention, advanced imaging, or other treatment options. Physicians are crucial in your health care, but for simple orthopedic concerns starting directly in PT can save you time and money. Quality of Care Despite the high charges being submitted, the reimbursement rate for those services by insurance companies is reducing. It takes more patients to meet profit margins and cover the costs of running and staffing the clinic. As more patients are forced to be seen by the same number of therapists, it often results in double and triple booking of appointments. Multiple patients for the therapist to manage at the same time equals less one-on-one time for you. Clinics either expect the therapist to run around barking orders or they use aides (individuals without a physical therapy degree) using preset programs directed by the therapist. In either case, the therapist doesn’t have time to invest completely in your care and often this means a “cookie cutter” treatment involving the most common exercises to treat a particular body region. These exercises are often performed with little supervision regarding form or response. In my opinion, this is helping ruin the perception of PT by the public, if you wanted a "cookie-cutter" treatment, you can find a youTube video giving you common exercises for "knee pain." Number of visits A standard PT prescription from a physician reads 2-3x/week for 4 weeks (or longer). In this traditional system, you can understand why multiple times per week may be needed when you may only be getting 15-20 minutes of one-on-one care in a 45-minute treatment session. Less personal attention will likely result in a longer time frame to get the results you desire! In my cash-based clinic, you are seen one-on-one and the number of visits is reduced as a result of this quality of care. Reducing the number of visits required to reach your goals, means less time away from work, family, and travel time to a clinic. The visit reduction is often a point overlooked when considering a cash-based PT clinic. For patients who have a $40-50 dollar co-pay or higher (instead of a high deductible plan), receiving care at a cash-based PT clinic 1x/week compared to 3x/week at a traditional PT clinic can be very similar in cost. So to the points already stated, would you rather receive high quality one-on-one treatment at a cash-based PT clinic 1x/week or be treated in a clinic where you are one of multiple patients the therapist is treating and you need to come more times per week? Insurance Regulations/Limitations Many insurance companies are moving to authorizations and pre-certifications in order to have treatment. Often, these tasks are performed behind the scenes by the organization performing the treatments by either the billing department, registration staff, or the therapists. Most often, the initial assessment is performed and this information is faxed along with information regarding the patient (name, date of birth, insurance policy #, etc.), to the insurance company. The information regarding your condition is reviewed and either a number of visits or a date range is approved for care. For example, this may be "6 visits are approved", "all visits are approved until a specific date", or a combination of both. When those 6 visits have been used or you are nearing the end of the approval date, the insurance company requires a full re-assessment of the patient and another form is faxed for additional approval. What does this mean for you? The time in that visit that the therapist had to treat you is now spent performing measurements and assessments that will unlikely change your treatment plan. And guess what? That time is being billed for! Furthermore, insurance companies often have policies restricting which treatments they will cover. This takes the power of treatment selection away from the therapist and places it on a group of policy makers at the insurance company. Do you trust your insurance company has your best interest in mind? Or do you think they are interested in saving money they have to pay or limiting beneficial care? Another detail with insurance plans to keep in mind: In 2018, 65% of major companies are offering high-deductible plans (HDP) as an option and 35% of employees selecting that HDP and paying less in premiums. link If you have selected a HDP, this means you pay a large out of pocket amount prior to insurance beginning to pay for medical costs at all. Often, unless you always meet your deductible or have complex medical issues, the cost of receiving therapy at a cash-based clinic is much lower than receiving care at a traditional clinic when paying to meet your deductible. So why cash-based PT at Goodman Performance Therapy? -Higher quality of care by receiving one-on-one treatment for your entire visit -Often leads to fewer overall visits -Unless you have great insurance or a lot of medical problems where you will meet your out of pocket maximum, it will likely save you money -No restrictions by insurance companies! At GPT, the best course of action and number of treatments are determined by need and the results you feel you are receiving each visit. -Removes productivity pressures on therapists in traditional clinics and puts the focus on your care! -Get access to personal cellphone number and email for improvement in care (no waiting until your next visit to ask a question, I’m a text/email/call away!) I’m proud to announce my achievement as a sports certified specialist (SCS). This is a board-certified clinical specialist designation by the American Board of Physical Therapy Specialties (ABPTS) of the American Physical Therapy Association (APTA) in the area of Sports Rehabilitation. Specialist certification formally recognizes physical therapists who have demonstrated advanced clinical knowledge and skills in a specific area of physical therapist practice. As a sports specialized therapist, I have demonstrated both advanced clinical rehabilitation knowledge pertaining to sports injuries and sideline management of acute sports injuries. As a part of the certification process, I took training out of state to become an Emergency Medical Responder (EMR) through the American Red Cross where I learned and demonstrated proficiency in advanced first-aid techniques and acute injury management. The whole process, a little over a year in duration also included intense studying in current research and rehabilitation techniques for all areas of the body to return an individual back to a high level of activity. (This explains my lack of blog posts for the last year!)
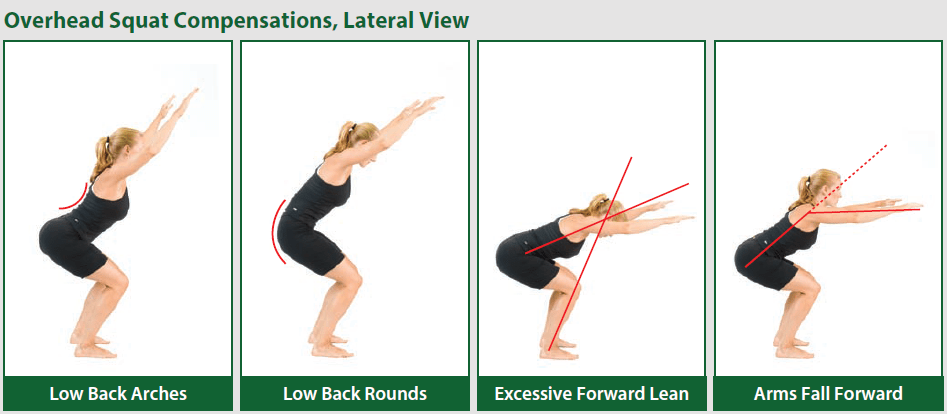
While I do get to add additional letters behind my name, it was never about this. This process was a great way to analyze strengths/weaknesses in my clinical practice and improve upon them. It also improved my use of evidence-based practice, which uses research to try to provide the best, most efficient treatments to help a condition. I believe in total, this process has allowed me to even further strengthen my skill set to provide the best treatments to help my patients the most. At the end of the day, that’s what it’s all about… helping those in need and forming trusting relationships. Whether you are an athlete, enjoy working out, or a desk jockey, the likeliness is you’ve experienced pain or discomfort at one point or another in your life. In many cases, these injuries will come and go in a relatively short time period and you don’t require treatment. But what about the injuries/pain that come and never fully recover or that keep coming back? This is where the skill of a physical therapist can come into play. Unfortunately, I think some people have misconceptions about what physical therapy is. Either they have had a negative experience in the past or feel “I don’t have time for therapy” as they think you need to devote multiple appointments a week for several weeks to treatment. I compare a physical therapist to a good lawyer. There are times where you might be in major trouble/conflict and need multiple visits to work something out, but other times you just need consultation and direction from time to time (or a tune-up). Also, just as all cars aren’t the same, all physical therapists aren’t the same. Unfortunately, there are still therapists out there using the “throw the kitchen sink at the patient and hope something works” technique. So where am I going here and how does this relate to functional movement assessment? A functional movement assessment has a patient perform multiple movements to systemically find the source of their dysfunction. This increases efficiency and effectiveness of treatment and there is a direct cause and effect relationship seen with activities/exercises! You see, I’m an impatient person, early in my career I never was really comfortable with the throw and wait technique. Just as you as a patient want to feel better, I as a therapist want more of an immediate result that I’m helping you. That’s why I get so excited about functional movement, dry needling, and cupping because when used together it can produce some of the quickest results I’ve seen as a therapist. Most of my patients need to see me 1-3 times to see major changes in their symptoms. The “homework” that you perform between visits work on exercises that are helping to build better movement patterns. As you get better with the movements, the stress on the injured area improves and your body has the ability to recover. Take the squat for example. Picture from www.thefitnesstraineracademy.org If you perform a squat and there is a flaw, this occurs for a reason and is likely putting extra stress on parts of your body. This can lead to INJURY and PAIN! These flaws may be the result of an injury or the cause of an injury. Just because you feel better after an injury doesn't mean all the effects of the injury are gone, hence why some people never feel "back to normal" after an injury. A functional movement assessment will break down the squat to determine why you are moving incorrectly and give you exercises that are components leading towards correcting these flaw(s). As your exercises progresses, your ability to perform a proper squat should also progress. Moving better means less stress on your body and your body is better at working as a machine. You should see a noticeable change not only in your ability to squat, but if addressing the appropriate mechanisms, YOUR SYMPTOMS! The original source of dysfunction, when optimized, becomes the exercise you need to build on to continue improving/maintaining the change. It’s the ultimate cause and effect relationship.
Contact me to discuss your personal functional movement assessment! Cupping therapy, although part of ancient Chinese medicine, was thrust into the limelight during the Rio Olympics. Although many of the athletes were being treated with cups, the American swimmers came out with circular red and purple marks which were visible on their skin. The announcers were obsessed with pointing out what the marks were and trying to explain the benefits of such treatment. New stories popped up on the internet claiming cupping was “pseudoscience”, “superstition”, and just the “latest fad” with pictures showing horrific burns. So what gives?
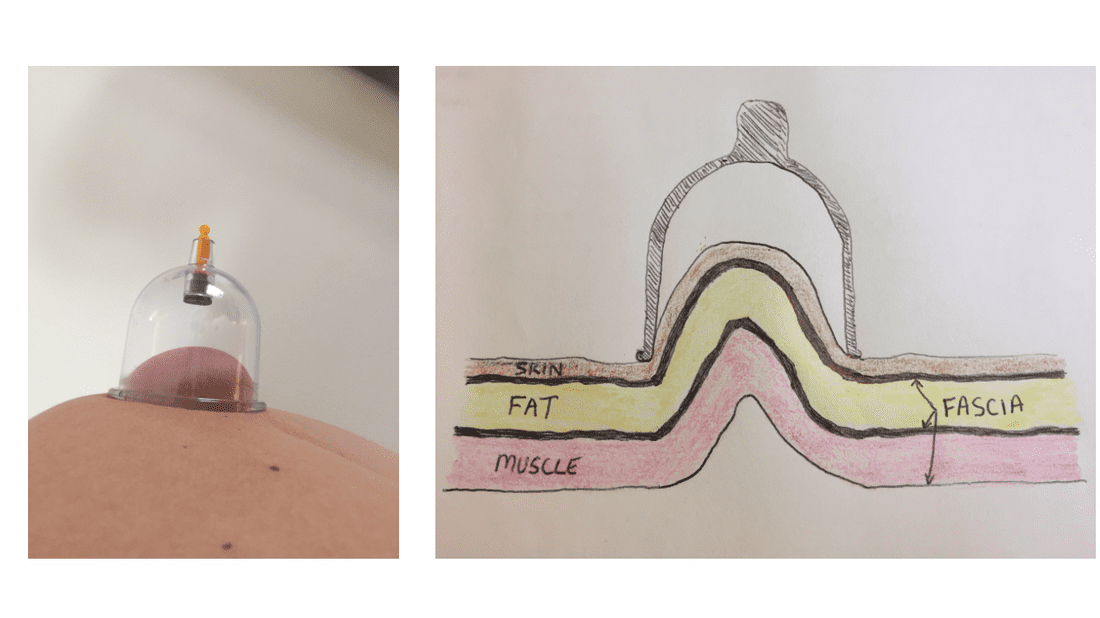
Let’s start by talking about what cupping therapy is. Cupping therapy involves placing a cup, which can be made out of different material ranging from plastic to glass. The general premise involves placing negative pressure under the cup forming suction. This can be achieved again through various means, but the most common is by a pump or by heating up the cup with fire just before placing on the skin. Although lighting something on fire is definitely more dramatic than adding a couple pulls to a plastic pump, I just don’t see the additional benefit of risking catching the clinic on fire, so I choose the plastic pump. Next, just as needling can be termed wet (with medication) or dry (without medication), cupping can be termed wet or dry. Wet cupping involves a form of bloodletting (cutting the skin and applying suction over the wound to suck out the bad, stagnant blood)-WHAT!?!? Umm no, no, no. Don’t get me wrong, if it works for you, great, but for some reason the “do no harm” vow that we take as medical professionals somehow feels broken when you slice open your patient just to watch them bleed. So let’s move on the the type of cupping that I perform, the dry version. Dry cupping again does NOT involve bleeding as a primary goal. The suction under the cup is thought to have many benefits, including: stretching tissue and fascia, increasing circulation and healing, and reducing pain just to name a few. The main reason I use cupping is for the stretching tissue effect, think of it like a deep tissue massage with much less time and effort. Where massage attempts to push through the layers to stretch the body, lengthening the tissue similar to rolling out dough with a roller, cupping pulls the tissue upward into the cup taking out the slack and providing a stretch (see pic above). The range of motion and flexibility gains after a simple treatment of cupping can be immediate and quite noticeable. Cupping techniques can vary according to the goal of treatment, but can involve simply placing the cups on the body and removing, moving the cups around once they are in place, or performing movements with your body while the cups are in place. So about the marks that the cups leave. They look like absolute torture right? So what does cupping feel like and how about those marks after treatment? When the cups are in place, think of an intense/effective stretch in the area targeted and then once the cups are removed, you tend to feel an immediate improvement in ease of movement and range of motion. The marks produced following may be a little sore to push on, but generally are not painful. They actually look much worse than they feel, with the patient not realizing they are even there after the treatment unless viewed. So prior to cupping, make sure you aren’t attending a wedding in a strapless dress and getting your neck/shoulders cupped! So why should I come to have cupping treatments performed with you instead of purchasing the $30 kits off Amazon and performing myself? First, when cupping is performed without training, serious bodily harm can occur if performed incorrectly! Also, just as with many other treatments, cupping is part of an overall treatment plan. Are the results permanent alone, probably not. After starting with a proper assessment, cupping can be combined with dry needling, stretching, or strengthening activities to target not only the symptom but the source. This is how you see results come your way. Do I have you interested……
Often I’m asked, why did you become a physical
therapist? I did not grow up thinking I always wanted to be a physical therapist, in fact like most kids, I was fascinated with planes and a pilot was probably what I said the most. As a son of a father who is an engineer, I did know what I didn’t want to be. You see, I was a hyper kid growing up, one that could never sit still, and the thought of sitting behind a desk at a computer in an office for 40 hours per week seemed dreadful. My father has dealt with low back pain and leg pain as far as I can remember. Frequently as a child, he asked me to walk on his back to try to help with his pain or he had mom massage his legs because of muscle spasms. He began having significant difficulty walking across the room, which led to his back surgery. It was hard for me growing up seeing him wanting to be involved in the games of baseball or basketball in the backyard, but either hurting too bad to attempt it or if he did, being laid up for a week recovering. I began going to his physical therapy appointments with him and quickly learned this is what I wanted to “do when I grow up.” The post I linked above is of major importance to me. Reading it alone is powerful, but looking deeper into the meaning is where I think it truly hits home. Often people thank me for “fixing” them, but I don’t view myself as a fixer or that I have this remarkable “gift”, I see myself as very passionate about what I do and like every physical therapist I like to help help people reach their goals. Sure there are treatments that require me doing something to you, but all in all, it’s just a step in the process of teaching you how to return to the things you want to do. A step to get me out of the picture and allow you to manage your symptoms or get rid of them all together. I want to get you back to spending more time and energy toward the ones you love or the things you love. It all comes back to why I got into therapy, helping dads get back to playing with kids in the backyard or kids returning to the sport they love. If you think I can help you reach your goals... Maybe you have back pain and are considering a technique called dry needling, but you’re not really sure what that means or what a treatment might entail. All you’ve heard was a co-worker raving about the relief they obtained after a treatment and that made you interested. You have tried other treatments….rest, medication, imaging, possibly physical therapy, or the dreaded I’m going to fix myself looking up things on the internet… (sticking with the OH MY theme on the blog), but your symptoms are still there. Let’s discuss more about dry needling.
Dry needling is a technique which uses solid filiform needles, which are often called acupuncture needles. This needle is designed for one time use and is usually a very thin stainless steel. Confusion usually creeps in over the fact that dry needling uses acupuncture needles. It’s important to point out acupuncture and dry needling are completely different, they both use the same needles but the location and purpose is vastly different. Acupuncture is generally based on qi, an energy form that travels in the body along meridians and treatment is attempting to rebalance this energy. Dry needling is based on scientific knowledge and anatomy which attempts to treat pain and trigger points by releasing the body’s natural hormones and chemicals. The term “dry” comes from the fact that the needle does not contain medication. Dry needling treatments vary depending on the desired effect, but may vary from a quick in and out of the needle to leaving multiple needles in up to 30 minutes. Electrical stimulation can be used to enhance the effect in many cases. I know, hooking up electricity via alligator clips to needles stuck in my body!?! WHOA, I don’t know if I signed up for this right? Most people have had electrical stimulation or even TENS treatments if you’ve experienced pain in the past. When receiving these treatments, you are using the same electrical current, but instead of needles you are using a sticky electrode that goes on the surface of the body. Where higher levels of electricity are needed to get through the layers of tissue when using an electrode, the electricity needed to stimulate a needle is MUCH less because it’s located directly in the effected structure. It’s the equivalent of watering the entire yard with a sprinkler hoping to hit the flower bed, when you can take a watering can and directly water the flowers. Much better results in less time! Treatments can result in significant pain relief and muscle relaxation, which when combined with the proper exercise can yield large gains. Large gains allow you to return quicker to THE THINGS YOU WANT TO DO! Do I have you excited yet? Dry Needling - My Experience
When I mention Dry Needling to most, the look of shock and horror usually fills their face. Maybe it's because I use the term needles, yes plural, which is a new concept to most. Here's how I got to my first experience... It was Sunday September 27, 2015, I was playing in my rec league hockey game. As I skated toward the center of the ice, a player heading full speed hit me head on. The collision was hard, happening so quickly I couldn’t even attempt to protect myself. I ended up leveled on the ice, with a concussion and the worst neck pain I’ve ever experienced. Six months off the ice dealing with concussion symptoms: nausea, headaches, visual problems, and head pressure combined with continued neck pain. My treatment path included visits to the doctor, manipulations to my neck, vestibular-orthopedic physical therapy, and neurological eye exam/treatments. Stretching, massage, ultrasound, strengthening, and vision exercises that you perform until you are nauseous. NO FUN! While the concussion symptoms gradually improved, the neck pain did not, while frustration continued to grow. In April 2016, I took Sue Falsone’s Dry Needling and Cupping training. For those that don’t know, when Physical Therapists go through training, this means you are basically a human guinea pig practicing every technique on each other throughout training. She asked for a volunteer to demonstrate techniques on the neck, this was my chance. My neck pain had increased from sitting in class and changing into so many different positions. Ten needles in the back of my neck and head and my pain was gone, the pain I had been experiencing for months, it was gone! And there it was, I was hooked and wanted to bring this powerful tool to others. So the big question... was it horrible to get stuck with needles? Not at all! Most of the needles I had no idea if they were in or out. Were a couple of needles sore going in, sure, but compared to the pain I was experiencing, this was nothing! Do I have you excited? Contact me to schedule an assessment! |
AuthorRyan Goodman is owner of Goodman Performance Therapy LLC and the Team Physical Therapist for the Columbus Blue Jackets with experience in Orthopedic and Sports Medicine Injuries. Archives
November 2018
Categories
All
|



 RSS Feed
RSS Feed